Heart Disease - Nutrition
Heart Disease Resources: Basics | Symptoms | Diagnosis | Dogs | Cats | Treatments | Medications | Nutrition | Forms
Optimal Nutrition for Pets with Heart Disease
While diet alone is usually not the sole treatment for heart disease, nutrition tailored to your pet’s heart condition may help slow the progression of heart disease, minimize medications required, and improve quality of life. In certain forms of heart disease (diet-associated dilated cardiomyopathy, for example), diet can even help reverse heart disease.
The nutrition goals recommended by your veterinarian will be specifically tailored to your pet and his or her condition. Whether your pet needs to gain weight or lose weight, increase muscle mass, or minimize fluid retention by eating a low-sodium diet, talk to your veterinarian or a board-certified veterinary nutritionist about the best diet for your pet. It’s also important to discuss appropriate treats for your pet and safe and effective ways to give medications.
Your veterinarian, veterinary cardiologist, or veterinary nutritionist might also recommend specific dietary supplements, such as fish oil or taurine. Please speak with your veterinarian before adding any supplements to your pet’s diet as they could have serious side effects or interact with your pet’s medications.
You can help your pet’s heart from early in life. Be sure your pet is eating an optimal diet made by a well-established manufacturer that meets all of the World Small Animal Veterinary Association's guidelines. To learn more about selecting the best diet for your pet, please visit Cummings Veterinary Nutrition page – Petfoodology – which provides fact-based information on pet nutrition, including “Questions You Should Be Asking About Your Pet’s Food”.
Nutritional Goals
-
A key goal for the nutritional management of heart disease is to maintain optimal body weight and muscle mass.
Ideal body weight is important for dogs and cats with heart disease – they shouldn’t be too thin or too overweight. Body condition can be assessed using the Body Condition Score chart for cats and dogs which assesses the amount of fat a pet has on a 9-point scale, where 1 is very thin, 9 is obese, and ideal for healthy pets is between 4-5. While the ideal score for healthy pets is 4-5, it may be beneficial for pets with heart failure to aim for a body condition score of 5-6. Owners should check their pet’s body condition score and monitor their weight regularly. Your veterinarian can help you if you’re not sure that your pet’s body condition score is where it should be.
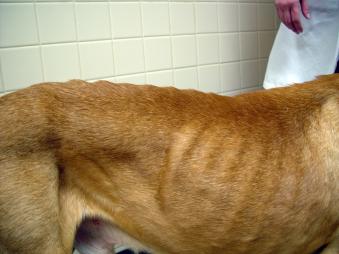
Muscle condition score is separate from body condition score since a thin pet can have normal muscle and overweight pets can have muscle loss. Muscle loss (also called cachexia) is very common in pets with heart failure.
You can assess your pet’s muscle condition score using muscle condition score charts for dogs and cats and using this video from Cumming’s veterinary nutritionist Dr. Lisa Freeman: Muscle Condition Score: A Critical Part of Patient Assessment
Your veterinarian can also help you determine your pet’s muscle condition score.
Many pets with heart failure will not eat as much (called hyporexia) or will be pickier or have different eating patterns (called dysrexia) as compared to when they were healthy. This can be an important factor in the weight and muscle loss that occurs. A complete loss of appetite (called anorexia) usually indicates a problem with either control of your pet’s heart disease or medications, and a trip to the veterinarian is recommended to find the cause. Maintaining your pet's interest in food is a tricky yet important task, but there are several tips to achieving this – see our section on “How to deal with a picky eater”.
While it is important to make sure animals are not too skinny, they should not be too heavy as this can make their symptoms worse. It burdens the heart to carry around extra weight and being overweight can also worsen difficulty breathing. A special diet may be prescribed for your dog or cat to help manage the heart disease as well as to gradually achieve their optimal body weight.
If you are unsure what your pet’s optimal weight is, please speak with your veterinarian to help craft a nutrition plan that is appropriate for your pet. Weigh your pet regularly to ensure he or she stays at optimal weight. It can be helpful to buy a digital scale for pets or babies so you can track cats’ and smaller dogs’ weight at home.
-
Too much of some nutrients can worsen a pet’s heart condition.
Sodium
Take a quiz to find out if you’re sodium savvy!Sodium, or salt, can cause the body to retain water. This excess water is bad for pets with heart failure since they are already retaining too much fluid and have fluid build-up in the lungs, chest, or belly. Sodium can be in anything you give your pet – pet food, treats, table food, dental chews, rawhides, dietary supplements, or foods used to give medications.
Your veterinarian or a veterinary nutritionist will be able to recommend specific foods to feed your pet; Note that while some senior diets are low in sodium, other senior diets are actually very high in sodium, so talk to your veterinarian about what specific diet is recommended for your pet or see our diet lists for low sodium diets for dogs and cats. You can also see our tips on low sodium treats and medication administration.
Potassium
Excess potassium can also be detrimental to a pet with heart disease. Certain heart medications, such as spironolactone or an ACE inhibitor (e.g., enalapril, benazepril, or lisinopril), can cause the body to retain potassium. Usually this is a good thing, since low potassium is a problem that can happen in animals taking diuretics. However, if your pet has too much potassium (called hyperkalemia), he or she may appear weak or lethargic and could collapse. Your veterinarian will monitor your pet’s potassium level in the blood with routine bloodwork to be sure it stays at an appropriate level.It is also possible to cause nutrient excesses by giving your pet dietary supplements. View our information on dietary supplements for heart disease. Be sure to talk to your veterinarian before giving any supplements to your pet with heart disease.
-
It’s important for pets with heart disease to eat good quality, nutritionally balanced diet from a well-established manufacturer (see our section on selecting the best food for your pet) so they receive optimal levels of all essential nutrients.
If you are feeding a home-prepared diet and it was not formulated by a board-certified veterinary nutritionist, it is almost guaranteed to have nutritional deficiencies (and sometimes excesses) that can be harmful to your pet’s health. If you wish to feed a home-cooked diet, be sure to work with a board-certified veterinary nutritionist to ensure the diet is safe and healthy for your pet. You can find a veterinary nutritionist at the American College of Veterinary Internal Medicine (Nutrition).
Large amounts of treats or table food can also cause nutritional deficiencies. Treats and table food should make up no more than 10% of your pet’s diet to avoid deficiencies.
Pets with heart disease require a nutritionally balanced diet to support their overall health, just like any healthy pet. In addition, there are some nutrients that are especially important for pets with heart disease.
Important Nutrients for Pets with Heart Disease
Protein/Amino Acids
A pet with heart disease should not be put on a low-protein diet because this can contribute to muscle loss (cachexia), especially when pets have congestive heart failure. In fact, as long as pets with heart failure don’t have significant kidney disease, they may need a diet that has higher than normal protein levels.Some senior pet diets can be too low in protein, which should be avoided in pets with heart disease. While it is normally recommended for pets with advanced kidney disease to be on a reduced-protein diet (along with restriction of phosphorus and other nutrient modifications), pets with kidney disease AND heart disease pose a unique nutritional problem that requires consideration of the needs of both diseases. Be sure to discuss the best option for your pet with your veterinarian.
Potassium
Pets with congestive heart failure will require diuretics, such as furosemide, to treat fluid buildup. Diuretics like furosemide cause the body to lose excess fluid - a good thing for the heart - but potassium is also lost. Potassium is essential for regulating your pet’s normal heart function and heart rhythm.Pets on diuretics, especially at high doses or when multiple diuretics are given, may become too low in potassium – called hypokalemia. This can cause your pet’s heart to beat in an abnormal rhythm. Signs that your pet may not have enough potassium include weakness, lethargy, muscle cramps, reduced appetite, collapse, or even fainting. Pets with congestive heart failure will need to have their blood potassium levels monitored; and if low potassium develops, a potassium supplement may be needed, often combined with changes in drugs or a different diet.
Magnesium
In addition to causing potassium loss, most diuretics (like furosemide) also cause loss of magnesium from the body. Magnesium is essential for helping your pet’s heart to beat normally.If your pet becomes too low in magnesium (called hypomagnesemia), they may appear weak, depressed, or unsteady when walking. Low blood magnesium can also contribute to abnormal heart rhythms (arrhythmias).
Maintaining optimal body composition and avoiding nutritional deficiencies or excesses are the primary goals for pets with heart disease, but it can become more complicated if your pet has other medical conditions, such as kidney disease, gastrointestinal disease, cancer, or bladder stones. In these situations, it will be important to address both heart disease and your pet’s other issues. It can be helpful to work with a board-certified veterinary nutritionist in these situations.
-
In addition to the main nutritional goals in heart disease, there can be benefits of some nutrients given as supplements. Certain dietary supplements can be helpful but also can have side effects and risks. Therefore, it’s important to select them carefully and use the right dose. In addition, there is little regulation of dietary supplements for people or pets. Effectiveness, safety, and quality control are questionable in many supplements and some of these products can be harmful or completely useless.
We recommend using dietary supplements that have the logo of the United States Pharmacopeia Dietary Supplement Verification Program. This group tests human dietary supplements for ingredients, concentrations, dissolvability, and contaminants. ConsumerLab is another independent group that tests supplements – primarily human supplements but some pet products as well.
Speak with your veterinarian about which specific supplements have proven benefit for your pet, have low risk of side effects, and what specific brands are worth buying.
Combination supplements (a mixture of many different nutrients) can be more difficult to maintain quality control and to have optimal levels of each individual nutrient. Therefore, individual supplements are recommended.
Be sure to talk to your veterinarian before starting any supplement as there can be interactions with heart medications or certain supplements may be too risky to use.
Coming Soon – handout about specific brands and doses of dietary supplements that can be beneficial for dogs and cats with heart disease.
Taurine
Taurine is an amino acid which, if deficient, can cause a specific heart disease called dilated cardiomyopathy (DCM). This condition, when caused by a taurine deficiency, is most often seen in cats. Good quality, nutritionally complete and balanced commercial cat foods have plenty of taurine, but diets that are not complete and balanced (labeled for intermittent or supplemental use only), vegetarian diets, diets made by inexperienced manufacturers, or homemade diets can be too low in taurine. If your cat is diagnosed with DCM, the cardiologist will test your cat’s plasma and whole blood taurine levels to see if they are deficient. If your cat is taurine deficient, taurine supplements will be prescribed to help treat the disease.Dogs, unlike cats, do not require taurine in their diet if they have enough of the building blocks of taurine in the diet (methionine and cysteine). However, certain breeds, such as the Cocker Spaniel, Newfoundland, St. Bernard, English Setter, Labrador retriever, and Golden retriever, may require higher levels of the precursors (or some taurine) in their diet to avoid a deficiency. Lamb and rice diets, very low protein diets, and high fiber diets in these predisposed breeds may make it more likely for them to develop a taurine deficiency and heart disease. If your dog is diagnosed with DCM, your veterinarian or veterinary cardiologist might measure plasma and whole blood taurine levels or recommend taurine supplementation.
Taurine can also have some mild benefits even if your pet isn’t deficient. It acts as an antioxidant and can help with contraction of the heart muscle.
L-Carnitine
Carnitine is a nutrient that is important for energy production in the heart muscle. Most dogs with dilated cardiomyopathy do not have a deficiency of carnitine but a family of Boxers was diagnosed with carnitine deficiency, so we sometimes recommend L-carnitine supplementation for Boxers with dilated cardiomyopathy.In addition, L-carnitine may have some mild benefits in dogs with DCM (even if they don’t have a deficiency) by helping with energy production in the heart muscle.
Omega-3 Fatty Acids (Fish Oil)
Omega-3 fatty acids are a special type of oil that can help reduce inflammation in the body and reduce muscle loss (cachexia) in pets with congestive heart failure. Omega-3 fatty acids do not prevent heart disease as they might in people. This is because, in people, omega-3 fatty acids may help prevent coronary artery disease, which does not occur in dogs and cats.Fish oil is recommended for dogs and cats with congestive heart failure, especially those with reduced or altered appetite or any muscle loss (cachexia). Omega-3 supplements can also be used (in addition to appropriate medication) in the treatment of dogs with abnormal heart rhythms (arrhythmias). Fish oil is relatively safe but if your pet has a bleeding disorder or is already eating a diet high in omega-3 fatty acids, supplementation should be carefully considered with your veterinarian.
Fish oil may be purchased over the counter at almost all human pharmacies, but the dose and quality of the products vary widely. See our handout for specific brands and doses of omega-3 fatty acids.
Antioxidants
Antioxidants help to rid the body of harmful substances that cause damage to cells. In pets with congestive heart failure, these harmful substances are produced at higher levels while the body is also producing fewer antioxidants to combat the danger.Supplementing with antioxidants can help bring the body back into balance and lower the stress placed on the heart. Some antioxidants can be harmful and many products do not have good quality control, so be sure to talk to your veterinarian before starting any supplements.
Coenzyme Q10 (CoQ10)
Coenzyme Q10 is a substance produced naturally in the body that works as an antioxidant and helps the heart muscle cells make energy. There are no definitive studies evaluating coenzyme Q10 in dogs or cats with heart disease but there are some studies in people with dilated cardiomyopathy that suggest beneficial effects. -
While there are many claims about raw meat diets (both home-prepared and commercial), there are no proven health benefits. There are many proven risks, from nutritional deficiencies to bacterial contamination that can make you or your pet sick. The bacterial contamination (up to 48% of commercial diets in one study) is a particular risk for pets with heart failure, which are known to have immune function changes that could increase their risk of getting sick. We strongly recommend avoiding raw meat diets in all pets but particularly those with heart disease. For more information, read Raw Diets: A Healthy Choice or a Raw Deal? Raw Diets: Pet Owners Frequently Underestimate Human Health Risks, and Raw Pet Food Risks: A Research Update.
-
Talk to your veterinarian about the specific diet that would be most appropriate for your dog or cat. Diets that are low in protein should be avoided unless your pet also has severe kidney disease.
We’ve put together a list of low sodium diets that may be appropriate for a pet with heart disease. Your veterinarian can help you select a specific diet. Don’t assume the canned and dry versions of a diet will be similar in nutrient content. Different flavors of the same food can also differ widely in their nutrient content. Also, the nutritional profiles of diets can change a lot from year to year so be sure to check with the manufacturer or the HeartSmart website regularly to be sure the diet you’re feeding is still right for your pet.
Depending on the severity of heart disease, decreasing the amount of sodium in your pet’s diet can be beneficial. In pets with mild heart disease (those that are not showing any symptoms), only mild sodium restriction is recommended. If your pet has congestive heart failure, greater sodium restriction is advised.
Sodium from Treats and Table Food
While it is important to feed the most appropriate pet food given your animal's specific heart disease, its severity, and other medical issues, also remember that large amounts of sodium can also come from treats, table food, rawhides, dental products, supplements, and the foods you use to give daily medications.For any of these foods your pet eats, be sure they’re low in sodium and safe to give to your pet with heart disease. The handouts provide some good options. All foods in this list should be prepared without salt. You should only feed these treats in small amounts (these extra treats should provide not more than 10% of your pet’s daily calories). Adding too much "people" food or other treats could result in an unbalanced diet that puts your pet at risk for nutritional deficiencies. See our handout on low sodium treats for pets with heart disease here.
Nutitional FAQs
-
Maintaining optimal weight and muscle is a key goal of managing a pet with heart disease. This can be especially tricky because heart failure often causes pets to lose interest in eating. Hormone-like substances the body produces in heart failure reduce appetite and cause weight and muscle loss.
To entice a pet that is uninterested in eating, try giving smaller meals more frequently. Cats often prefer their food warmed. Dogs are less predictable but will usually prefer one temperature. Try seeing if your dog prefers their food warmed, room temperature, cold, or even briefly put in the freezer. You can also try feeding your pet from a different dish or even in different locations in your home.
If these changes don’t improve your pet’s appetite, it may be time to change the diet. Try switching how the food is presented – if your pet usually eats dry kibble, try a low sodium canned diet. If you do switch brands, make sure the pet food you switch to is made by a reputable and trustworthy manufacturer.
If you would like to cook a homemade diet for your pet, please consult a board-certified veterinary nutritionist who can create a balanced and complete diet for your pet (to learn more about the training and qualification of board-certified veterinary nutritionists, see the post on Petfoodology). A homemade diet that is missing essential nutrients could end up worsening your pet’s condition.
Finally, it is important to be aware that a complete loss of appetite (called anorexia) usually indicates a problem with either control of your pet’s heart disease or medications, and a trip to the veterinarian is recommended to find the cause.
Taste enhancers can help your pet eat his food more readily.
The addition of omega-3 fatty acids from fish oil supplements can also have mild benefits for appetite and maintaining muscle in some animals. For more on omega-3 fatty acids, see the dietary supplements section.
There are also two safe and effective FDA-approved drugs that are used to stimulate appetite in pets: Mirataz® (mirtazapine transdermal ointment) for cat and Entyce® (capromorelin oral solution) for dogs. Talk to your veterinarian about an appetite stimulant if your pet is not eating enough of her diet or if she won’t eat enough of the recommended diet.
-
It is critical for the successful treatment of your pet’s heart disease to be able to give all recommended medications regularly. But some dogs and cats can be incredibly skilled at avoiding their medications. With practice, patience, and creativity, you too can become a pro at pilling your pet.
Food Suggestions for Giving Medications
Some pets may take pills better if the medication is disguised in a treat. With any of these treats, you want to give the minimum amount of the treat needed for your pet to accept the pill. This will avoid unnecessary calories and nutrients. Also, it is important that those foods be low in sodium.For most pets, we recommend not putting pills directly in their food bowl as this could make them avoid their meals.
Some pill pouches or pockets sold in stores can be high in sodium and might be a bad option for pets with heart disease. Greenies Pill Pockets (dog peanut butter flavor; cat chicken or salmon flavors) are fine to use. Also, try to use the smallest size possible (ideally, the cat-sized Pill Pockets, even for dogs) and use as few as possible to avoid excess sodium. Check any other pill pouches to be sure the sodium level is ok (less than 100 mg sodium for every 100 calories).
For dogs, peanut butter is a good option as long as you check the label to be sure it is “unsalted” or “no salt added.” Otherwise, it’s likely to be high in sodium and not safe to use. Also, check to make sure that it does not contain any artificial sweetener such as xylitol.
A dollop of a low sodium canned food can be a treat to hide pills.
For dogs or cats, a small amount of home-cooked meat such as chicken or hamburger (made without salt) can be used to hide medications. Be sure to avoid deli/lunch meats and rotisserie chicken.
For dogs, try soft fruits such as banana, orange, melon, or berries. Avoid fruits like grapes and raisins as these can be toxic to pets.
If your dog has a sweet tooth, treats such as mini marshmallows, whipped vanilla cake frosting, or whipped cream cheese can be good for hiding pills. Just be sure to check that the sweet contains less than 100 mg of sodium for every 100 kilocalories.
If you decide to hide your pet’s pills in food, always be sure they are eating the food AND medicine. If your pet is especially sneaky, you might need to check their mouth and their bed after they’ve eaten to ensure they’re not hiding the pill.
For more tips on giving pills, check out our handout on treats and nutritional tips for pets with heart disease here.
Non-Food Alternatives for Giving Medications
First, if you are giving multiple medications at a time, try putting several smaller pills into an empty gelatin capsule. This way, you only have one capsule to give your pet instead of going through the ordeal multiple times. You can purchase these capsules from your veterinarian or online.Check whether your pet’s pills must be given with a meal or on an empty stomach to be most effective or minimize side effects. If you have questions, call your veterinarian. Also be aware that crushing pills or opening capsules can alter the absorption and effectiveness of some medications, so discuss these actions with your veterinarian first.
Try having your veterinarian or veterinary technician teach you how to give medications directly into your pet’s mouth at the back of their tongue. This method doesn’t involve any additional food or treats. A pet piller or pet pill “gun” can also make giving pills easier.
A compounding pharmacy may be able to make your pet’s medication in a flavored liquid or chewable form to make it more appealing to your pet. As cats are notoriously difficult to give pills to, a liquid form of the medication might be the answer. However, compounding can alter the effectiveness of some medications, and the drugs may have a shorter shelf life, so speak with your veterinarian first. In general, if you can give medication in the original formulation, this is preferred over compounding.
Once your pet has taken its pill, be sure to reward them with something they enjoy. That might be an appropriate treat, a favorite toy, or going for a walk. This will help your pet associate the pill with something enjoyable and make your pet easier to pill over time.
For more tips, see our Petfoodology post called, “Pill-Popping Pets”.
-
With hundreds of pet food manufacturers and thousands of pet foods to choose from, it can be incredibly challenging for pet food owners to select the best diet for their pet. For the owner of a pet with heart disease, this can be even more complicated.
Your veterinarian will be able to help you select the best diet for your pet and his or her condition, but here are several tips to ensuring your pet is eating right.
While commonly used, the ingredient list is one of the least useful and least objective ways to select your pet’s food. This is because the ingredient list doesn’t help us determine the quality of the individual ingredients or the company’s nutritional expertise or quality control. For more reasons on why you shouldn’t judge a pet food by its ingredient list, check out the Petfoodology post on the topic.
While looking at your pet’s bag or can of pet food, one thing to check is the nutritional adequacy statement. All pet food is required to have one – if this food is your pet’s primary diet, you want to make sure this statement does not say “This product is intended for intermittent or supplemental feeding only”, as these diets do not contain the minimum amounts of all essential nutrients, and your pet could develop deficiencies.
Beyond the bag, a much better way of evaluating your pet’s diet is determining whether it is meeting the World Small Animal Veterinary Associations guidelines which include ensuring the manufacturer employs qualified nutritionists to formulate their diets and adheres to strict quality control measures. Obtaining this information can be difficult and often requires a phone call to the brand in question. The Pet Nutrition Alliance also has a resource that compiles this information.
Your veterinarian will be able to recommend specific diets to support your pet with heart disease. For more information on selecting the best diet for your pet, read Petfoodology’s post “Questions You Should Be Asking About Your Pet’s Food”.
-
Recently, the FDA has issued statements about a possible link between certain pet foods and the development of dilated cardiomyopathy (DCM), a serious form of heart disease. DCM is usually an irreversible disease but some dogs with diet-associated DCM have improved with a diet change (and appropriate heart medications). While the exact cause of diet-associated DCM has not been determined yet, we recommend the following:
We recommend that you DO feed a diet:
- that meets the World Small Animal Veterinary Association Guidelines to help ensure it is nutritionally complete and balanced and made by a well-established company with strong nutritional expertise and rigorous quality control measures
- containing common meats, such as chicken or beef
- containing grains
- that is low in sodium (if your dog has heart disease)
We recommend that you DON’T feed a diet:
- based just on the ingredient list or the marketing
- containing at least 1 pulse (peas, lentils, chickpeas, beans) or potatoes/sweet potatoes in the first 10 ingredients or more than 1 anywhere on the ingredient list
- that is raw, vegetarian, or vegan
- that is homemade unless you work with a Board-Certified Veterinary Nutritionist™ to ensure the recipe is nutritionally complete and balanced (and you follow the recipe exactly)
For more information on diet-associated DCM, please visit Petfoodology’s posts on the topic:
- A Broken Heart: Risk of Heart Disease in Boutique or Grain-Free Diets and Exotic Ingredients
- It’s Not Just Grain-Free: An Update on Diet-Associated Dilated Cardiomyopathy
- Dilated Cardiomyopathy (DCM): Update, July 2019
- Diet-Associated DCM: Research Update
- Diet-Associated Dilated Cardiomyopathy: The Cause is Not Yet Known but it Hasn’t Gone Away